Addressing the production and supply chain complexity of autologous CAR-T cell therapies
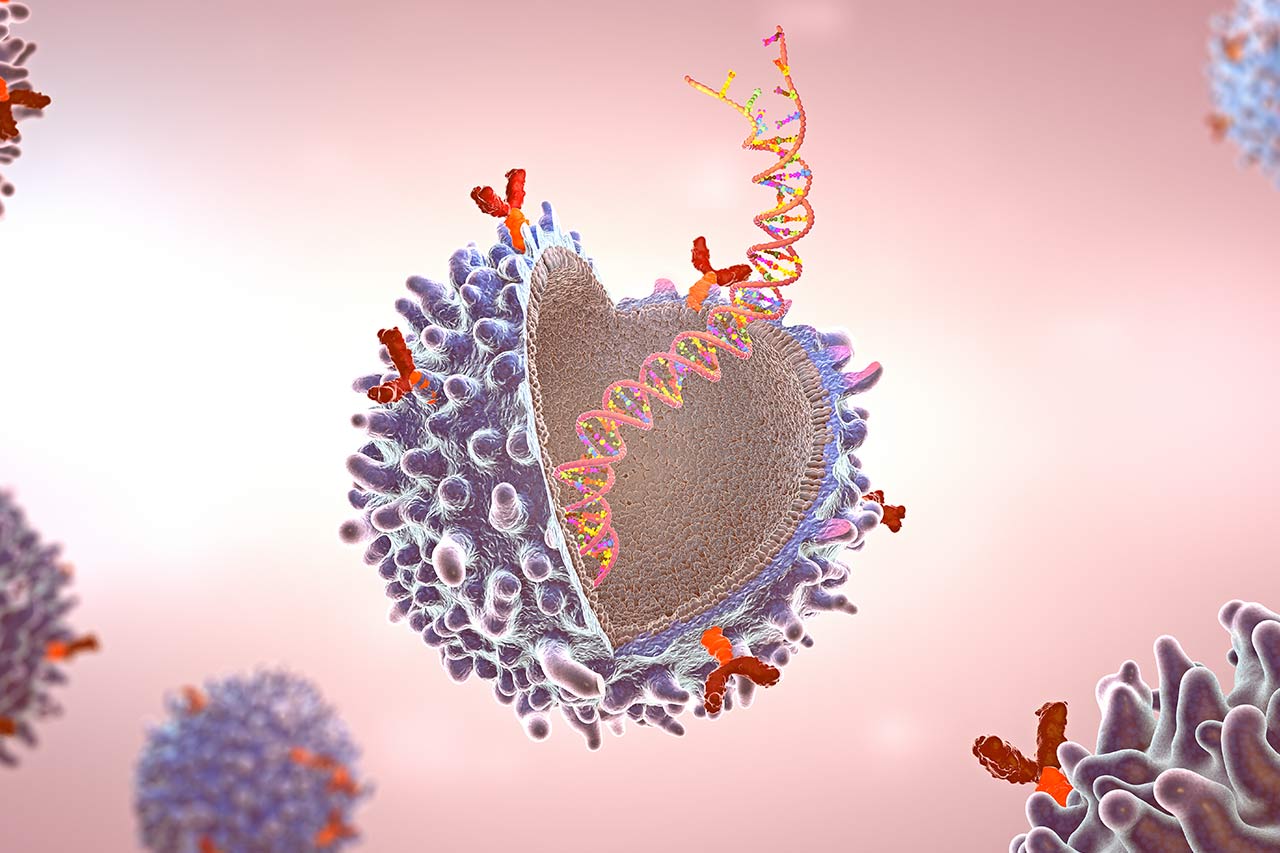
All the approved CAR-T cell therapies in the market today are derived from the patient’s own immune cells, thus they are autologous CAR-T cell therapies. These cells are collected, expanded, and manipulated in highly specialized laboratories to make them able to recognize cancer cells, after which they are infused back into the patient where they will fight the patient’s cancer cells.
This approach results in several constraints when compared to traditional medicines that can be mass-produced in an industrial setting and then shipped worldwide. Here for autologous CAR-T cell therapies, for each patient a new batch must be produced, requiring several steps to collect, transport, manufacture, qualify, and finally return the cells to the patients for infusion.
And even though this is a highly centralized process few economies of scale can be made as the model is not amenable to scale-up. Furthermore, complex logistics are required to maintain the cold-chain and keep the “collection to injection” times as short as possible. All this while maintaining the chain of identity for each individual batch.
This means that today the process requires 2 to 3 weeks, from collection to administration, but several approaches are being taken to reduce both time and logistical complexity, such as :
- Building more robust supply chains
- Decentralizing production
- Using allogeneic therapies that can be manufactured in large batches from unrelated donor tissues.
As more CAR-T therapies move from the lab to the bedside ensuring supply chain efficiency is critical to guarantee that patients receive their treatment on time and minimize risks. Many companies are working together with suppliers to ensure their operations are up-to-speed and can be scaled-up accordingly, often taking inspiration from the blood industry and other therapies that faced similar problems. Indeed, since the launch of Yescarta, Gilead has managed to reduce the turn-over time from 26/29 days in 2019 to 17 days currently all while expanding access to the therapy.
Part of these improvements in autologous CAR-T cell therapies are due to better supply chain platforms and logistics. Newcomers arose who specialize in providing such services to cell therapy manufacturers such as Vineti, TrakCel, Cryoport and others. These are able to integrate and connect all the pieces of the supply chain in one platform, from managing the chain of identity and custody, to scheduling of manufacturing slots and handling the logistics of collection and shipping to hospitals worldwide. All this while ensuring the sample have been maintained at the right temperatures, improving lead times and reducing the risk for both patients and manufacturers.
Automated cell therapy platforms for autologous CAR-T cell therapies
Another approach to meet demand and reduce complexity in the production of cell therapies focuses on automating the process and reducing the square footage required. Allowing installation at the point-of-care (PoC), in hospitals and clinics where they can be used by the medical staff. This measure avoids the need to transport the collected cells and final product to and from the manufacturing facility that can be hours if not days away.
In 2018, Lonza, one of the biggest CMO’s in the world, acquired Octane Biotech a company developing Cocoon®, an automated, scalable cell therapy manufacturing platform designed to be installed at the PoC. The Cocoon® is an end-to-end manufacturing platform for cell therapies that utilizes a single-use cassette system that contains the necessary reagents and consumables needed for the process, allowing for a closed automatized system. This means that the need for highly specialized personal can also be minimized, further reducing costs. Additionally, the system is scalable, allowing up to 10 cocoons to be attached to a tree-like system with each system having a footprint of on-square meter reducing the overall production surface needed.
Recently the company announced they have successfully treated the first patient with CAR-T Cell immunotherapy manufactured using the Lonza Cocoon® Platform at the Shega Medical Center in Israel. A landmark step to allow decentralization and manufacturing of CAR-T cell therapies at the PoC.
Shifting from autologous to allogeneic CAR-T cell therapies
Another way companies are addressing these issues is by shifting from autologous to allogeneic cell sources. In allogeneic therapies, cells are not derived from the patient itself but rather from unrelated donors that can be used to produce large batches to have an off-the-shelf-option that can be used to treat many more patients. This innovative solution reduces complexity and time for treatment administration, as these are immediately available and can be standardized.
Lately, we have seen a rise in the number of allogenic molecules in clinical trials. Among these, Allogene Therapeutics, is currently developing a platform with the potential to treat 100+ patients from a single manufacturing run, allowing for a drastic reduction of costs while also permitting product optimization since more time is available for manufacture. A major hurdle in allogenic therapies is the graft-versus-host disease due to the recognition of these cells as foreign. However, several strategies are being developed to minimize this side-effect, including further gene editing and new allogeneic cell sources.
| Autologous | Allogeneic |
| Pros | Highly compatible with patients’ immune systems. | Universal, “off-the-shelf” product, scalable potentially leading to cost savings. |
| Cons | Longer manufacturing times and costs. If the manufacturing fails this means the patient cannot receive treatment | Graft-versus-host disease Lower efficacy when compared to autologous |
| Trends | Development of automatic systems deployed at the point of care. | Further gene editing to reduce side effects and improve cell survival |
Table 1: Summary of the main pros & cons of autologous vs allogeneic CAR-T approaches and respective trends
Navigating the challenges of cell therapies and the impressive results of autologousbCAR-T cell therapies represent a real revolution for both clinicians and pharmaceutical companies alike. Many of the former approaches to manufacturing and supply chain need to be adjusted as we pivot from a “one-drug-serves-all” to patience-centric treatments and business models. New challenges will continue to arise in a field that we, at Alcimed, will for sure continue to follow.
About the author
Joel, Senior Consultant and Quentin, Project Manager in Alcimed’s Healthcare team in Switzerland